Oligodendrogliomas are a rare type of glioma, which are tumours that originate in the brain.
That long, complicated name refers to the fact that oligodendroglioma cells originate from cells called oligodendrocytes, which cover and protect nerve fibers. The name comes from the Greek words oligo, which means few, and dendro, which means trees or branches, because oligodendrocytes look like they have little branches reaching off them.
How rare are Oligodendrogliomas?
Only about 3% of all primary brain tumours are oligodendrogliomas. They’re most common in adults between the ages of 20 and 40 and can occur in children. It is estimated only around 1,200 people a year in the United States are diagnosed with an oligodendroglioma, but the incidence of these tumours has increased recently.
What are the symptoms?
The symptoms of an oligodendroglioma depend on the size and location of the tumour, and can be mistaken for a stroke at first.
As the most common symptom is seizures; 60% of patients will experience a seizure before diagnosis. Other less common symptoms include: headaches, changes in behaviour or personality, and weakness or paralysis.
How is someone diagnosed with an oligodendroglioma tumour?
Diagnosis usually starts with a physical examination by a physician who will further discuss your symptoms and do testing to identify any concerning changes. They look at things like coordination, speech difficulties and vision or memory changes, followed by a brain scan (usually a CT scan and then an MRI), and finally surgery, which is the only definitive way to know what type of tumour it is.
How are oligodendrogliomas treated?
Oligodendrogliomas can be either grade II (slow growing) or grade III (fast growing/malignant). Treatment decisions are based on what type it is, how big it is, where it is, and how healthy the patient is.
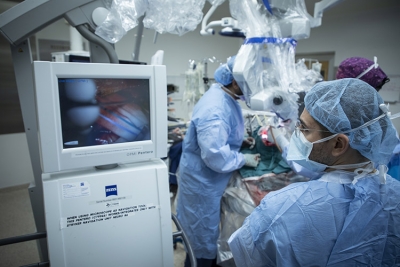
The first treatment option is usually surgery; the goal is to obtain tissue to determine the tumour type and to remove as much as possible. It is often challenging to be able to remove the whole tumour, but with modern technology and skilled surgeons, it is now more often possible. Following surgery, or in cases where surgery is not possible, treatment options include radiation and chemotherapy.
What is the survival rate?
Patients with Oligodendroglioma have a higher survival rate than most other malignant brain tumours. As with treatment options, life expectancy after diagnosis depends on many factors, but an important one is the extent of resection. Around three quarters of all oligodendroglioma patients will still be alive five years after diagnosis.
Patients with grade II tumours are likely to live over 10 years after diagnosis but those patients with grade III tumours have a shorter life expectancy.
Oligodendrogliomas do have a high recurrence rate, and they increase in grade over time.
What’s the future of oligodendroglioma treatment?
Because oligodendrogliomas are rare, research into their specific treatment has been limited. Donor support is essential when it comes to better outcomes for oligodendroglioma patients. It was donations from the community that helped equip The Ottawa Hospital with cutting-edge technology and advances such as the CyberKnife, incorporation of advanced awake mapping techniques into brain tumour surgery and 5-ALA Fluorescence Guided Surgery using the fluorescence-guided microscope — which have changed the way we do brain surgery.
These changes have led to The Ottawa Hospital having higher survival rates for brain cancer patients than anywhere else in Canada.

