In a time where the public must stay home, essential workers are making their way to The Ottawa Hospital each day. They are here to care for the sickest in our region because after all, other illness and injury won’t take a backseat to COVID-19.
Doctors, nurses, and essential support staff walk through the hospital doors with one goal in mind: to make sure each patient has the best possible care. In the midst of a global pandemic and public fear, these hospital team members also have to find their own way of caring for themselves, their families, and remaining healthy through the difficult times.
They are the calming voice for each patient, whether it’s a surgeon performing lifesaving surgery for your loved one, a nurse administering chemotherapy treatment, or an orderly sharing a smile and kind words to a patient who isn’t able to have visitors at this time.
These are the stories from the frontlines of The Ottawa Hospital.
Preparing for the pandemic
Preparing for COVID-19 is not just about ensuring that The Ottawa Hospital is ready, it’s also about organizing the entire Champlain region of hospitals. That’s where Dr. Andrew Willmore, Medical Director, Department of Emergency Management at The Ottawa Hospital comes in.

Dr. Willmore is also the Incident Commander for the Champlain Health Region. He’s been helping, in partnership with the City of Ottawa, to prepare for an influx of patients who are expected to require hospitalization as a result of COVID-19. That preparation began about four years ago by creating an Incident Management System (IMS) within The Ottawa Hospital.
“This allows us to create mechanisms to flip into an incident mode, which allows us to reorganize how the hospital functions and when we should escalate to a higher level,” explains Dr. Willmore.
When the pandemic started and The Ottawa Hospital was tasked with coordinating the response in the region, an IMS structure was applied to the rest of the region. “This allowed us to implement changes to our care delivery models like opening the COVID-19 Assessment Centre, Care Clinics, as well as a regional staffing and logistics distribution model to ensure departments that are struggling are supported,” explains Dr. Willmore.
“I am so humbled by this role. I have a long day, I look around, and I see everyone who has had just as long of a day. The talent we have in house and regionally is beyond my expectations. It’s really a powerful thing to see come together at the end of the day.”- Dr. Andrew Willmore
The key has been working collaboratively with Ottawa Public Health to flatten the curve. The response of the community has given Dr. Willmore and his team the lead time to implement the plan without the hospitals becoming overburdened. “We’re sprinting to preparedness. We are looking at the whole system as a region. If you don’t have someone zooming out, then it’s very easy to trip over each other.” There’s no tripping in this collaborative effort.
With a long road still ahead, Dr. Willmore stops to reflect on the work he and his colleagues at The Ottawa Hospital are doing during these unprecedented times. “I am so humbled by this role. When I have had a long day, I look around, and I see everyone who has had just as long of a day. The talent we have in house and regionally is very inspiring, and absolutely everyone is engaged. It’s really a powerful thing to see come together at the end of the day.”
“Despite physical distancing, I’ve never seen a community come together like this before.” – Kim Hargreaves
Nurses rally together
Kim Hargreaves is a nurse in the medical day care unit specializing in blood cancer. She and her colleagues administer chemotherapy and supportive care for those with blood cancers, such as Leukemia, Lymphoma, Multiple Myeloma, and MDS.
Even during the COVID-19 pandemic, that care must continue for these patients. “In medical day care, we support each other 100 percent. Everybody pitches in,” says Kim.

Kim explains that nurses are being redeployed from other areas of the hospital to provide care to these patients. “Nurses from clinics whose patients are able to meet with their doctors virtually are cross training to come and help our team on the frontlines.”
This dedicated nurse, who is celebrating 31 years at The Ottawa Hospital this year, says all the community support is really helping the front-line team. “When you see those signs, you straighten up your shoulders and you know you’re needed and appreciated no matter how tired you are.” Kim continues, “We are not rushing around like in the Emergency Department or ICU, but we’re providing continuity of care.”
In all her years of nursing, Kim has never been so inspired by what she’s witnessing during this pandemic. “Despite physical distancing, I’ve never seen a community come together like this before,” says Kim.
Back from retirement
Within three hours of calling The Ottawa Hospital, Robin Morash was rehired and she was back in her scrubs within days helping patients.
After 33 years as a nurse at The Ottawa Hospital, with many years in management at the Cancer Centre, Robin was two years into retirement when she felt compelled to return. “We were hearing day in and day out just how busy the teams were, and I wanted to help my community.”

Robin is doing just that by working at the COVID-19 Assessment Centre along with many colleagues and community partners. She says this is exactly what she trained for as a nurse and why she needed to return to work. “It’s a part of who we are. The idea of just sitting back and watching others scurry around, just isn’t us (nurses).”
Nurses ‘get it done’
Alongside Robin at the COVID-19 Assessment Centre is Joselyn Banks, a former clinical manager with The Ottawa Hospital who had just retired in December 2019 after a nursing career that spanned 35 years. When the pandemic hit, she cancelled a trip to Florida and contacted the hospital to find out how she could help.
“I looked at my colleagues and friends — I’m very proud of them. I’m very happy to have helped, in at least this little way.” – Barb Bijman
“For me it was just knowing our community needs help. Knowing the colleagues and friends I have at The Ottawa Hospital must be working crazy hours and I just wanted to be able to come back to help whoever, whenever, and in whichever capacity that I could,” says Joselyn.

Joselyn has been putting her skills to work at the COVID-19 Assessment Centre since the day it opened. She says it’s reassuring to know their work at the centre is having a positive impact. “We’re hearing feedback from many of our colleagues back at the campuses that we’re doing great work and helping to keep people who want to get swabbed out of the Emergency Department. So that’s great as well.” The centre has so far diverted more than 9,000 patients away from the Emergency Departments.
It’s not lost on Joselyn the magnitude of the situation, but she says this is what nurses do. “For us, I think we’re passionate, we’re caring—we’re nurses. We’re doers. Let’s get up and get it done. Let’s go.”
The sacrifice of coming out of retirement

It’s not an easy decision to come out of retirement at a time like this. There are sacrifices–Jennifer Smylie knows that all too well.
Jennifer says she made the conscious decision to return to work, knowing she wouldn’t be able to have close contact with her elderly mother. But as a lifelong nurse, it’s what she needed to do. “There is some risk to it, but we’ve done things like this throughout our careers. We weighed the risk and decided this is the right thing to do.”
The veteran nurse, who spent more than 30 years at The Ottawa Hospital, and was most recently a manager in the cancer program before retiring, stepped in to work with the screeners.
Screeners are on hand to greet anyone who enters The Ottawa Hospital during the COVID-19 pandemic. In order to keep everything organized and safe, Jennifer answered the call. “I didn’t hesitate, and I thought this is the right thing to do,” says Jennifer.
She explains it’s an important role to keep patients and staff safe. “We make sure anyone who enters the hospital answers the screening questions and they are safe to enter. It’s very busy, but we’re trying to be very compassionate with everyone we screen.”
Retired nurse proud to be back
After 34 years working in the ICU at The Ottawa Hospital, Barb Bijman retired from nursing in 2017, but kept her license. Little did she know that she’d need it to lend a hand during a global pandemic.
The decision to return to the frontlines meant giving up time with her grandchildren and elderly mother, but she had to do it. “It’s a nurse thing—we go to help. That’s why so many of us decided to come back from retirement,” says Barb.

As her voice cracks from emotion, she acknowledges it’s a stressful time for everyone, both healthcare workers and the public — yet she couldn’t imagine being anywhere else than providing support at the COVID-19 Assessment Centre. “I’m so proud of The Ottawa Hospital, everything it has done. It’s a really good place. I was looking at it from the outside in, at times like the bus crash and now. I looked at my colleagues and friends—I’m very proud of them. I’m very happy to have helped in at least this little way.”
Team at 3D Printing Lab steps forward
As members of The Ottawa Hospital’s 3D Printing Laboratory watched how COVID-19 was unfolding in China and Europe, they saw how some parts of the world were facing dramatic equipment shortages. That’s when Dr. Adnan Sheikh, Director of the 3D Printing Laboratory, reached out to Dr. David Neilipovitz, Department Head of Critical Care to offer help.
Since then, the 3D printing team has been able to think creatively to help protect colleagues who will be caring for patients critically ill from COVID-19. That team also includes Dr. Olivier Miguel and Dr. Leonid Chepelev, both research associates.
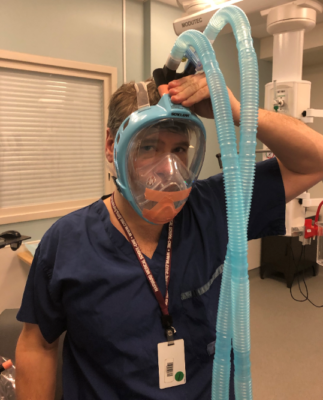
Dr. Neilipovitz has played a key role in testing these designs in advance, allowing The Ottawa Hospital to be innovative during challenging times. “Thanks to our 3D team, they allow us to think outside the box and find us solutions to help our patients,” says Dr. Neilipovitz.
It’s a time where colleagues are helping colleagues. “We have developed and adapted multiple designs for personal protective equipment (PPE),” says Dr. Chepelev.
Dr. Chepelev adds the hospital’s 3D printing lab is producing as much quantity as it can handle right now. “We have used our 3D printers to produce the necessary parts such as smaller connectors, respirator mask parts for PPE, ventilator prototypes.” It’s a truly collaborative effort explains Dr. Chepelev, “As printing takes time, the team has been able to use the printers to prototype devices which we then pushed out to production at the various Ottawa 3D printing sites with hundreds of volunteers, or where possible to local plastics manufacturers.”
The best part of all, notes Dr. Sheikh, is that this all came about organically. “Colleagues helping colleagues—having an open mind and being willing to integrate what we can contribute. Assessing the gear and testing it out to make it reality.”
Changing ways for palliative care
Dr. Miriam Mottiar is an anesthesiologist and a palliative care physician at The Ottawa Hospital. While significant changes have been implemented for her work as an anesthesiologist in the operating room, including suiting up with PPE, it’s the changes she’s seen as a palliative care doctor that pull at her heart.
The COVID-19 crisis has made it very different for patients and their families. “Patients no longer have their family members at their bedside because of the visitor restrictions,” explains Dr. Mottiar. In order to provide that compassionate care, Dr. Mottiar and her team are still trying to help patients and their families connect during these difficult times.
“We are facilitating a lot of phone calls and video chats between patients and their family members. We’re also having more patients request to go home for end of life care, where they may not have been asking for that before, because at home they can have their loved ones with them.” In order to accommodate, Dr. Mottiar works with community partners to help with those requests from her patients, when possible.
She acknowledges these are challenging times for her palliative patients, as it’s not until the final hours of life that a family member can join their loved one in person. She adds, “It breaks my heart a bit as a human and a physician because we’ve had to change the way we practice due to the very significant concerns we have about the virus spreading in our community.”
I.T. up for the unprecedented challenge
It was an unprecedented task for the technology team at The Ottawa Hospital. Within three-and-a-half days, the COVID-19 Assessment Centre, a remote, out-of-hospital clinic where patients could be assessed by a healthcare provider and tested for COVID-19, needed to be ready for patients. They made it happen.
Jim Makris, Manager of Networking and Voice Services, says it meant preparing two separate buildings to be connected back to The Ottawa Hospital. “We had to set up a network connection back to the hospital, build a network at the new facility, install wireless access, and we had to deploy our phones as well.” Bottom line, Jim’s team had to make sure the front-line healthcare workers had the same access to The Ottawa Hospital as their colleagues at each campus. “Normally it would take a month to get a facility like this up and running. We did it in two days.”

Swift action made the centre operational. Next Stephen Roos, Manager of Client Services, stepped in with his team to make sure equipment was brought in, set-up, and running efficiently. “In addition, experts trained in Epic, the hospital’s Health Information System (HIS), arrived to provide the nurses on site with the training they needed to make sure all patients’ information was entered into Epic so that they could be made available to patients via a secure process using MyChart. That was an important piece in this process,” adds Stephen.
Both Jim and Stephen acknowledge this was a true partnership between the City of Ottawa and The Ottawa Hospital. It was the city which brought both power and internet access to the buildings allowing the hospital’s team to take over.
The two men are quick to add their unit is humbled to have the opportunity to support the front-line workers. “Yes, things came together really fast for our I.T. team and we worked a few really long and hard days, but the fact the front-line workers are going into work each day, caring for patients—what we did is nothing compared to what they do,” says Stephen.
Keeping the supplies on track

Roman Medzhitov is a Material Management Supervisor at The Ottawa Hospital. It’s a crucial role for him and his team these days.
Roman is responsible for all material supplies, from tissue to linen to personal protective equipment that go through the Civic Campus. He’s in charge of each unit and delivering supplies. “Since the arrival of COVID-19, supplies are the biggest demand,” acknowledges Roman.
Knowing that patient and staff safety is of utmost importance, Roman’s role has changed from a weekly check-in with units, to a 24-hour cycle of communication. “We reconnect every 24 hours to ensure departments are equipped with what they need to keep staff and patients safe. Together, we take an inventory and review the most important items and supplies.”
The bridge from research to patient trials

When Irene Watpool started hearing about all the different COVID-19 research starting up at The Ottawa Hospital, she knew there would be a need for a bridge between research and the patients. Currently there are more than 50 projects, 14 that received funding thanks to generous donor support.
Irene has been a nurse for over 30 years, and has worked on clinical trials for 23 years with The Ottawa Hospital’s research team. As the program manager for research in the Intensive Care Unit, she acts as the liaison between research and the patients, and knows the gentle way to approach each person and family to discuss patient trials.
“The role that I have taken on, along with my colleague Rebecca Porteous, is to be the one point of contact for in-patients in the COVID-19 studies,” explains Irene.
Some studies involve having medications, blood work, while others require nasal swabs. Irene and her colleagues are trying to coordinate every detail so that the patients aren’t impacted too much. There are two types of trials involved, one that could potentially benefit the patient through medication or treatments, while other trials focus on future patients and better understanding the disease.
“For more than four weeks, I’ve been approaching almost every COVID-19 positive patient that comes in to see if they would participate in research. It’s actually quite surprising because these people are sick, and the swabs are uncomfortable but the patients are so gracious and willing to participate in research. It’s amazing,” says Irene.
Irene adds patients seem to understand the importance of their role and the research. “They are being very altruistic. You really have a sense they don’t wish the disease on anyone and they’re willing to help.”
As for her team’s role, Irene says she can’t imagine being anywhere else. “I feel privileged to be involved in this.”
While we all face uncertainty with each coming day, there is a calming reassurance knowing our front-line healthcare workers are harnessing their knowledge to care for all patients during these challenging times. It’s that care which we will look back on someday, and it will only be then that we realize how instrumental each role was when our community was in need during these unprecedented times.
The Ottawa Hospital is a leading academic health, research, and learning hospital proudly affiliated with the University of Ottawa.




