Published: April 2026
Read time: 4 min
Published: April 2026
Read time: 4 min
On Christmas Day 2023, Jody Stang fell to the kitchen floor. When his brother stopped by for a visit, he found Jody sitting with his back pressed against the cupboards — unable to get back up on his own. This wasn’t like him.
Jody served 31 years in the Canadian Armed Forces, including six operational tours in Afghanistan, Bosnia, Cyprus, and Croatia. He was in peak shape: he walked regularly, cycled long distances, and kept up with weight training.
But in the months leading up to the fall, something felt different. His balance was off, his legs seemed weaker, and for the first time in decades, Jody missed the local Remembrance Day ceremony — a day that is deeply personal to him. Soon, he could no longer drive, and even walking short distances was a challenge.
What started as numbness in his baby toe was clearly becoming something much more serious.
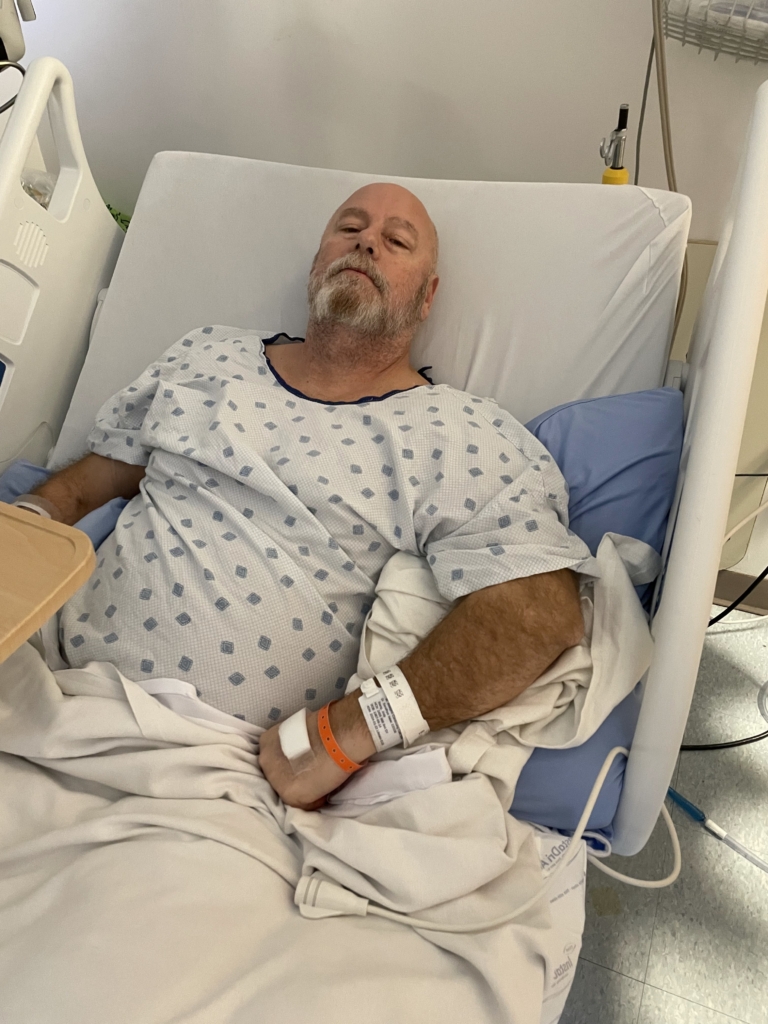
Searching for answers
The day after his fall, Jody called an ambulance and was taken to the Cornwall Community Hospital. After some initial tests, physicians arranged for him to be transferred to The Ottawa Hospital. With one of the strongest neurology teams in the nation, The Ottawa Hospital is the only centre in the region equipped to provide the advanced neurological care he needed.
Doctors initially suspected MOG antibody-associated disease (MOGAD), a rare autoimmune disorder where the immune system attacks the protective layer of the nerves in the brain, spinal cord, and optic nerves, which would explain Jody’s muscle weakness and numbness.
He was started on high-dose steroids and later returned to Cornwall for continued care and rehabilitation. But instead of improving, Jody continued to decline. By then, he had lost nearly 85% of the sensation and motor function in his legs and was dependent on a wheelchair.
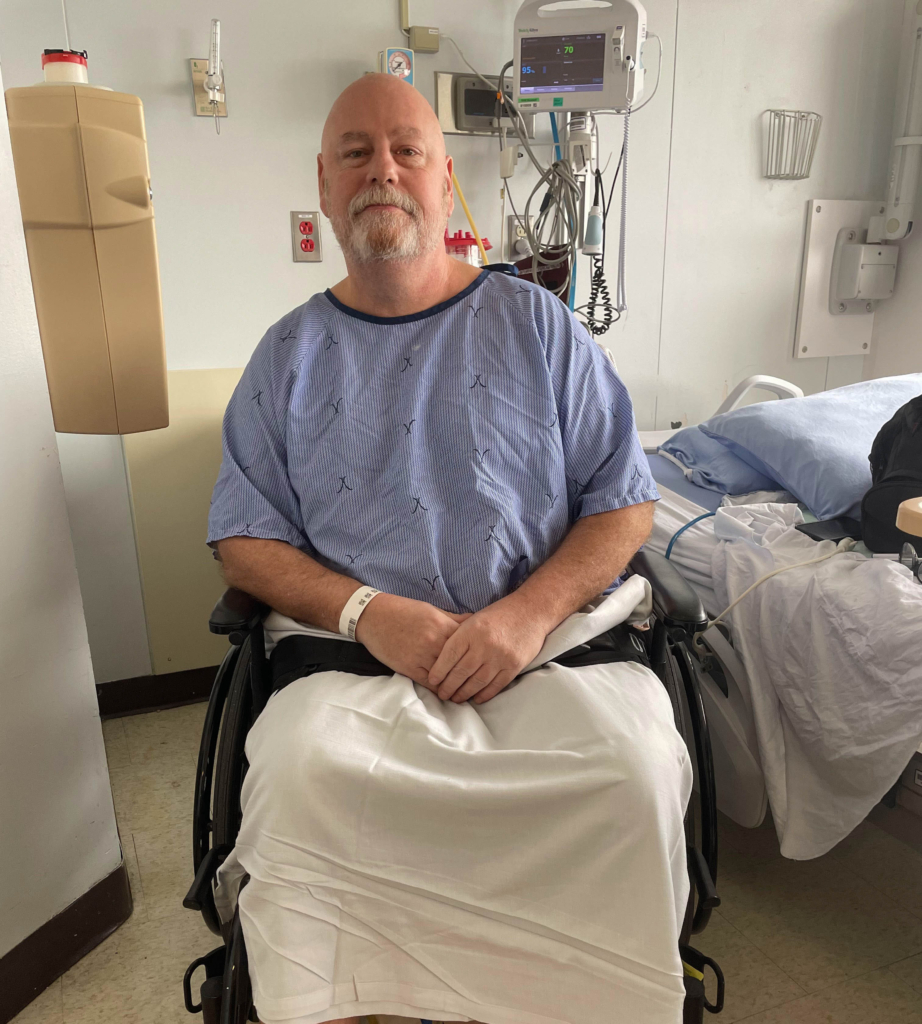
An unexpected diagnosis
Dr. Giulia Fadda, a neurologist and specialist in MOGAD at The Ottawa Hospital, saw Jody for a follow-up appointment in early February. Immediately concerned, she arranged for him to return as an inpatient to the neurology unit.
Five rounds of plasma exchange followed — a treatment option for more advanced stages of the disease. Still, there was no improvement.
His medical team ordered more imaging, including an MRI and PET scan, which revealed subtle changes near Jody’s L1/L2 vertebrae. The scans raised suspicions, and Dr. Safraz Mohammed, neurosurgeon at The Ottawa Hospital, recommended a biopsy.
The results revealed what no one had expected.
“Symptoms can mimic other neurological conditions, which makes early detection especially challenging.”
— Dr. Safraz Mohammed
Jody had the highest grade of brain tumour, called glioblastoma, but instead of being in his brain, it was in his spinal cord, which is incredibly rare.
“Spinal cord glioblastoma is incredibly uncommon,” explains Dr. Mohammed. “Symptoms can mimic other neurological conditions, which makes early detection especially challenging.”
The reality of spinal cord glioblastoma
Glioblastoma is one of the most aggressive forms of cancer. But glioblastoma in the spinal cord is exceptionally rare and complex to treat — fewer than 200 cases have been documented in reported literature worldwide. This type of cancer is often devastating, typically leading to paralysis as it infiltrates the spinal cord.
The diagnosis explained the numbness and weakness in Jody’s legs, and he grappled with the news that life-long paralysis was now inevitable. But nothing could have prepared him for the news that came next.
For a cancer like glioblastoma, average life expectancy is usually measured in months. Jody was told he likely had less than one year to live.
“I was shocked,” says Jody. “But through all my years as a soldier, I’ve learned to take difficult circumstances one day at a time. You can take the man out of the army, but you can’t take the army out of the man.”
It was then that Dr. Mohammed presented an option that offered some hope.
Surgery remained a possibility. While it couldn’t reverse the damage already done, removing the tumour offered the best chance of extending Jody’s life.
“By the time we confirmed the diagnosis, Jody had already lost most of the strength in his legs,” says Dr. Mohammed. “But based on the location of the tumour, we had a surgical opportunity to remove the tumour completely, which we can’t often do with glioblastomas of the brain.”
Meet Neurosurgeon Dr. Safraz Mohammed
Canadian-first surgery lights the way
Under Dr. Mohammed’s care, Jody underwent a groundbreaking surgery with a fluorescence-guided microscope, funded by generous community donors.
Several hours before the operation, Jody drank a liquid containing 5-aminolevulinic acid (5-ALA), a compound that accumulates in cancerous cells but not healthy ones. Under a specific blue wavelength of light generated by the microscope, the malignant glioma in Jody’s spine glowed a fluorescent pink.
“While we use this technology in brain tumour surgery all the time, it had never been applied to the spine in Canada,” says Dr. Mohammed.
Prior to Jody’s procedure, The Ottawa Hospital was the first centre in Canada to adopt widespread routine use of 5-ALA in tumour surgery. Today, the hospital is considered a national leader in fluorescence-guided neurosurgery.
Now, with the cancer cells clearly visible, Jody’s surgical team was able to remove all the tumour tissue with extraordinary precision, while preserving as much surrounding healthy spinal cord as possible. The surgery was a success and offered Jody something he hadn’t expected after his diagnosis — more time with loved ones.
All about fluorescence-guided surgery and 5-ALA
Ongoing treatment and recovery
Surgery was only the first step. In the weeks that followed, Jody underwent 30 rounds of radiation therapy alongside oral chemotherapy to target any remaining cancer cells and reduce the risk of recurrence. The chemotherapy continued for six months — the standard regimen for glioblastoma.
Regular follow-up appointments and scans also remain an essential part of his care. For Jody, who uses a motorized wheelchair, telehealth has made that ongoing care far more accessible. “Telehealth allows patients like Jody to be monitored and supported from their own home,” says Dr. Garth Nicholas, Jody’s primary oncologist. “We can adjust treatment, check on side effects, and answer questions without the added strain of regular travel.”
Advances in technology at The Ottawa Hospital are not only transforming surgery — they’re reshaping how care continues long after the operating room.
Hope for the future
Though his road to recovery hasn’t been without its challenges, Jody remains in good spirits. There was a time when he believed he would not see another Christmas. After being told he had approximately one year to live, Jody began preparing for the end — arranging a burial plot and purchasing a tombstone.

Today, more than two years later, his latest scans show no evidence of cancer.
“I’m incredibly thankful,” says Jody. “For the care I received from my healthcare team and for the chance to have more time with friends and family.”
Jody’s outcome is a testament to what’s possible when innovation, expertise, and donor-supported technology come together.




