The “seeds” are one millimetre by three millimetres, a third the size of a grain of rice, and made of platinum. These tiny seeds, created by researchers at The Ottawa Hospital, improve the CyberKnife robot’s accuracy in detecting and delivering precise doses of radiation to tumours in the brain and body.

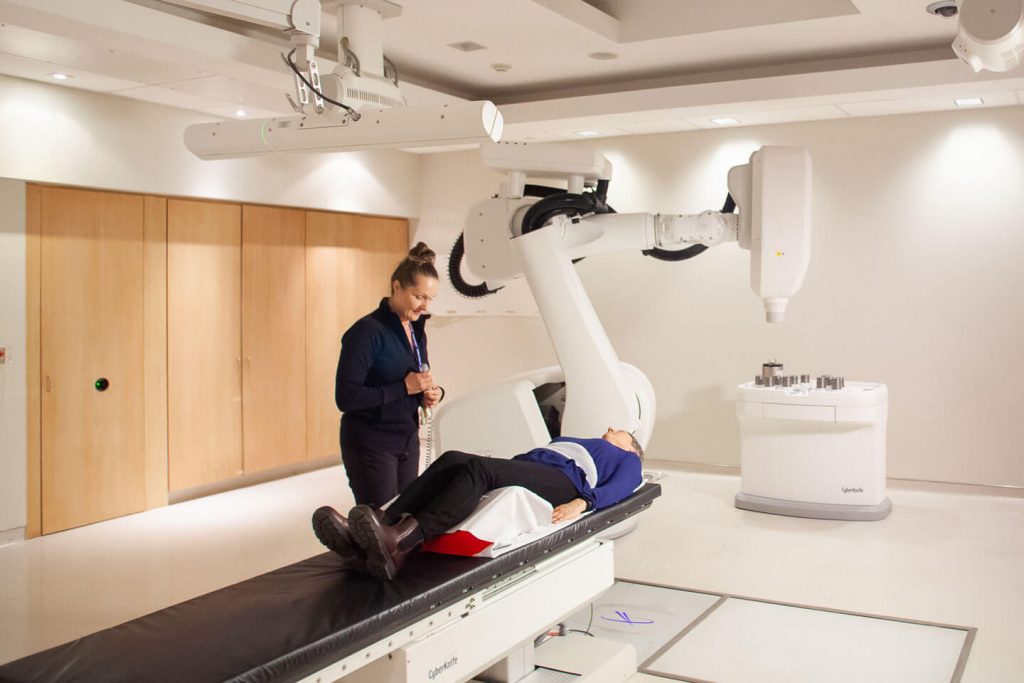
CyberKnife uses X-rays and complex precision software to track and focus radiation directly to the tumour. With accuracy of less than a millimetre, there is virtually no radiation spill over to normal tissue. As a result, patients have much better responses to this type of treatment compared with traditional radiation where a larger area is targeted.
“Because CyberKnife delivers a high dose, it’s considered similar to surgery without using a scalpel, so no blood loss, no pain, no ICU stay, or recovery time,” said Dr. Vimoj Nair, one of the radiation oncologists trained to prescribe CyberKnife treatment.
Ninety percent of CyberKnife treatments are for malignant or benign brain tumours, but CyberKnife’s image guidance system can also treat tumours in organs that move constantly, such as the lungs, kidneys, liver, prostate gland, and lymph nodes. It can precisely align the radiation beam to the tumour even when it moves. But radiation oncologists and researchers at The Ottawa Hospital are refining techniques to further enhance the performance of this state-of-the-art technology to improve patients’ outcomes. These techniques are ultimately changing radiosurgery practice.

“One unique thing that the CyberKnife research team at The Ottawa Hospital has come up with are in-house designed platinum MRI-compatible seeds that can be implanted around the moving tumour,” said Dr. Nair, who is also a clinician investigator at The Ottawa Hospital and an assistant professor at University of Ottawa. “We can see the tumour and the seeds better on the MRI, and the CyberKnife software can detect and track the motion of the tumour with the help of these seeds. The robotic arm of the CyberKnife matches the target motion to treat the tumour more accurately while the patient breaths normally.”
The Ottawa Hospital is one of the first centres in North America to use these platinum seeds. In the past, oncologists used tiny gold seeds, but they were difficult to see in the MRI sequences used to view the tumour. This made the treatment planning less accurate. Dr. Janos Szanto, medical physicist, and Dr. Len Avruch, radiologist (now retired), were the initial brains who took platinum wire (otherwise destined to be jewelry), cut it into minute pieces, and then put through a sterilization process to ensure the seeds were appropriate for insertion into the human body. It worked. They were visible to the naked eye, more visible in an MRI than the gold seeds, and could be detected by CyberKnife.
“The benefit of this technique is we see both our target and seeds more clearly together, which provides the best use of advanced imaging and improves the accuracy,” said Dr. Nair, who called the discovery novel research and application that positions The Ottawa Hospital very favourably on the world stage.
Dr. Nair was the first author on the research paper published about the platinum seeds. He said that researchers and clinicians are continually sharing innovative CyberKnife techniques they’ve developed, like this one, at conferences and with other health centres across Canada and globally. In September 2018, he gave presentations on The Ottawa Hospital practices on clinical uses of CyberKnife at a conference in India.
“We can see the tumour and the seeds better on the MRI, and the CyberKnife software can detect and track the motion of the tumour with the help of these seeds.”
Read more about the history of the community-funded CyberKnife at The Ottawa Hospital.
The Ottawa Hospital is a leading academic health, research, and learning hospital proudly affiliated with the University of Ottawa.




